Health workforce
A well-managed quarantine facility which operates with a primary healthcare foundation can have positive impact on the healthcare system.
By establishing onsite health support with qualified staff, residents can have many health concerns assessed and managed reducing the number of people requiring transfer to acute health services.
As presented in this section, a number of key elements need to be established to ensure a clear governance structure for the quarantine service, including arrangements so that the system is not dependent on individuals, and there is coherent incorporation into the broader command and control structures and decision making points and escalation processes.
At Centre For National Resilience (CNR), Howard Springs Quarantine Facility (HSQF) there was a multidisciplinary group of staff who contributed to facility services and resident care. With a mix of registered health professionals and administration officers, the Pod Teams (resident-facing staff) interacted daily with all residents onsite.
The Tele Wellbeing Teams maintained an online connection for residents and were often their first contact with the quarantine service through the pre-arrival teams.
The Operations Team completed many functions across the site to ensure the service ran smoothly such as stocking PPE, and assisting with resident arrivals and departures.
These and many other teams were guided and supported by a strong Leadership Team who were often adapting site processes and strategies at short notice in reaction to changing disease trends, community outbreaks and CHO Directions.
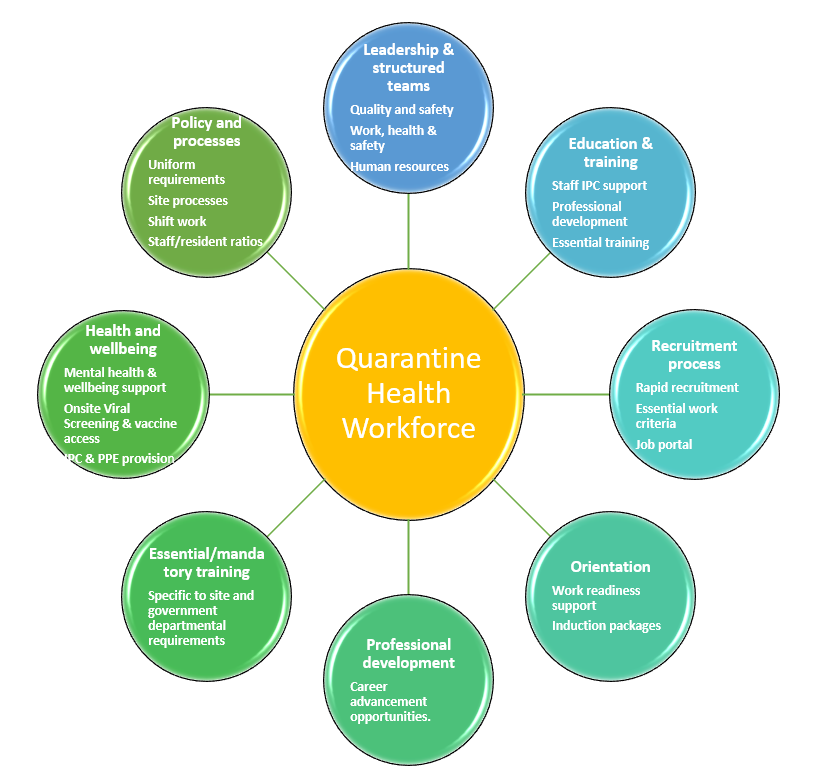
The CNR had a rigorous set of policies that aligned with the CHO Directions to ensure their staff were supported in their roles and remained COVID-19 safe onsite. All staff were required to record their arrival and departure onsite, be fully COVID-19 vaccinated, and undergo daily COVID-19 self-swabbing as determined by the CHO Directions. Regular education and training sessions were held for all staff and nursing-specific programs were established to support the junior nursing workforce to develop their clinical skills and knowledge.
The site practiced with an assumption that all residents entering quarantine could be COVID-19 positive and enforced staff and resident self-responsibility for being COVID-19 safe in their practices. Training of staff to be work ready incorporated a full 2-day orientation with hands on practice of infection prevention and control (IPC) and personal protective equipment (PPE) implemented onsite.
This section focusses on the health workforce for a quarantine and isolation service. The models presented are based on those implemented at CNR and have been updated in accordance with current research and feedback from CNR staff and leadership teams survey responses.
Access the full resource for Section 3 Health Workforce
Individual sections for resident care are presented with the information below.
A strong and resilient quarantine facility Leadership Team is required to collaborate across the pandemic response teams, remain current with public health emergency strategies and guide their staff teams to achieve their best for the residents.
Working in the front line of a pandemic response is challenging and the workforce needs to have confidence in the sites Leadership Teams decision making and processes.
This section provides a comprehensive overview of the Leadership Team structures in a quarantine facility. It is noted this is based on a primary health approach with many health professionals forming the core leadership roles. The teams working across the facility are divided into groups representing their core functions for resident care, site infrastructure, resident supportive processes and administration.
The approach to team structures in alignment with site responsibilities will be presented by unpacking each of the leadership areas. It is noted that certain teams have also been presented in other sections of this resource including the Medical Service Leadership team in Section 5 Health Wellbeing and Clinical Care.
Access the full resource for Section 3 Leadership Team Models
Operations team members are embedded across the site to manage core tasks including site deliveries, organise resident requirements such as welcome packs, personal hygiene packs and children’s packs, maintain PPE accessibility across all resident and training zones, and coordinate and assist with resident arrivals and departures.
The operations team consists of many staff who are trained onsite for specific roles and they are a core contributor to ensuring the facility runs safely and efficiently. This includes the Resident Services team who specifically oversee the arrival and departure process for all residents onsite.
Access the full resource for Section 3 Operations Team
Nurses contributed greatly as frontline workers across the COVID-19 pandemic response in acute, primary health, and emergency response teams and in quarantine and isolation facilities.
The presentation of the Pod Team outlines the main roles and responsibilities of the nursing staff onsite. Nurse Leaders managed specific quarantine service areas as demonstrated under the Clinical Services Leadership Model and operated under the instructions of the Director of Nursing. These leadership areas included the education and training team, infection prevention and control lead, site quality and safety, nurse managers for Pod Teams across repatriation, domestic, international and humanitarian residents, and the Tele Wellbeing Team (this nurse was positioned with the Operations Team).
A number of nurses recruited to work in quarantine and isolation are considered junior in relation to their time since registration and level of work experience and thus it is vital to provide support programs to assist these new nurses to develop their nursing skills, knowledge, confidence and competence.
This section presents the roles of the nurse managers and their focus areas for the quarantine facility. This includes an overview of the different programs in place to support nursing teams working in a quarantine and isolation facility.
The Specialist Team provides an important service for the quarantine facility adding another layer to the resident’s health and wellbeing support.
This team consists of a Nurse Manager and Social Worker as Team Leaders with a full team structured in accordance with resident numbers and their anticipated needs. This includes physiotherapists, occupational therapists, additional social workers, drug and alcohol nurses, mental health nurses, a trauma nurse practitioner and welfare support. Additional Specialist Team members are strategically located with the Tele wellbeing services and consist of a mental health nurse and welfare services.
A comprehensive overview of the Specialist Team’s role and responsibility has been presented in Section 5: Health, Wellbeing and Clinical Care. This includes the team model, interpreter roles and referral systems.
The Tele Wellbeing team (TWBT) focus is enhancing the well-being or emotional wellness of residents, this service provides a contact point for residents via online/phone services.
The TWBT were trained in Psychological First Aid (PFA) providing them with the skillset to promote and support residents in maintaining their mental health. They are not the same as a TeleHealth team which provides a level of health service online by health professionals but rather a team established to assist residents on their quarantine journey and promote resident wellbeing. This team assist with a number of core resident management tasks including the resident pre-arrival process, contacting residents during their stay for routine wellness checks and advising of important occurrences such as departure confirmations, viral screening or changes to the times when meals will be getting dropped off.
The Tele Wellbeing team does not provide any health advice and instead refers residents onto the Pod Teams (where they have access to registered nurses), Specialist Team, Medical Officers or to external health services if required. The Tele Wellbeing team are advised to have a registered nurse to assist with the triaging of difficult calls and all Customer Support Officers have a mental health first aid certificate which will provide skills they can implement online.
The Pod Teams have regular daily interaction with residents and are positioned as the first point of contact for any healthcare needs that may arise for residents in the zone (additional wellness contact points occurring with the Tele Wellbeing team).
The Pod Teams consist of nurses and administrators, and each has specific roles and responsibilities for the care of residents, they are the main staff group residents will connect with. This team steps into action on the arrival of residents with any pre-arrival information corresponded via the Resident Services and/or Tele Wellbeing team.
This section provides an overview of the main responsibilities of the Pod Team onsite and in caring for residents in quarantine and isolation.
The Department of Infrastructure Planning and Logistics is a public sector, government team who covers lands and planning, monitors roads, transport and safety, oversees government buildings and infrastructure and undertake planning and consultation where required.
The department aims to drive the sustainable, economic and social advancement of the NT through:
- land use and transport planning
- infrastructure investment
- effective logistics supply chains.1
They were a core group at the Centre for National Resilience with a multi focussed role that included:
- Weekly Zone, Maintenance and Forward Planning Meetings
- Site maintenance inclusive of structural maintenance and building repairs (including residents’ rooms).
- Management and maintenance of site gardens.
- Mitigation of environmental risks (in the NT this includes cyclones, flooding and heat waves).
- Site upgrades in accordance with site needs, such as bringing in additional de-mountable buildings.
- Working alongside work health and safety managers to identify and address any site infrastructure or design which may pose a health risk.
- Infrastructure improvements
Staff recruitment for the quarantine facility should be overseen by an Emergency Response Workforce (ERW) Hub as this team can manage the application process and organise possible candidates.
During the early stages of the establishment of Centre for National Resilience a rapid recruitment process was undertaken for administration roles which involved the screening of a large group of applicants for this specific position. Applicants were interviewed in groups of up to 12 people at a time allowing an overview of the core responsibilities to be presented and for candidates to ask any questions.
On the completion of each group interview successful applicants were identified and notification sent back through the ERW Hub who followed up the final contract process with successful candidates. All were then contacted by the sites Education Team to attend orientation.
A full outline of the ERW Hub responsibilities has been presented in Section 6: Northern Territory COVID-19 Response.
All staff need to attend a structured orientation program prior to commencing their roles to ensure they are confident and safe as a frontline worker in a quarantine and isolation facility.
A staff survey conducted with CNR staff demonstrated that 85% of staff were working with COVID-19 positive residents which demonstrates a high-risk environment. Despite this risk, 95% of staff felt safe from contracting COVID-19 onsite. A large contributor to this feeling of safety was due to staff preparation with a focus on infection prevention and control and personal protective equipment requirements.
Site orientation is managed by the Education Team and is coordinated with the Emergency Response Workforce Hub which manages staff recruitment so the site is aware of who and how many people to expect. For effective management of the Education Teams time it is recommended that orientation is initially offered weekly (for example every Monday/Tuesday) for new staff and then fortnightly as staff numbers are acquired.
This section provides a guide to developing a staff orientation as well as a basic set-up plan to prepare an initial staff group to care for 200 residents.
Access the full resource for Section 3 Workforce orientation
The Education Team needs to be located onsite and lead by nurses with additional qualifications in public health and education and training.
This team are situated to represent the facility goals, strategic plans, policies and processes to prepare new staff with the skills and knowledge they require to safely carry out their roles.
The Education Team core functional goals include:
- Prepare and support a (COVID-19) safe workforce.
- Provide professional development opportunities.
- Assist and monitor staff to meet mandatory training expectations.
- Review education and training provision for a quality assurance cycle and evidence of professional development outcomes.
This section of the pandemic quarantine facility guide will present recommendations for IPC education and training, professional development and mandatory training for staff.
Access the full resource for Section 3 Staff Education and Training
The health workforce are representing the facility and therefore need to ensure professional behaviours and appearances are maintained.
Staff should always be professional and culturally appropriate in accordance with their role, duties and the community/resident cohorts which they are working with. This also aligns with being safe in relation to infection, prevention and control expectations. These expectations will support residents and staff to feel safe, confident and comfortable whilst respectfully recognising that they are working with people from a range of diverse backgrounds.
In alignment with the expectations on staff attire and behaviours the site has a responsibility to:
- Implement positive workplace culture programs strengthening organisational culture and ethical, safe, respectful and compassionate workplace.
- Provide employees with flexible work options to help them meet their personal, cultural and family needs and obligations.
A policy to clearly present these expectations is required, and this may be the policy in place by the Department of Health or a new site policy may be introduced. This section presents a number of recommendations for site policy formation on staff attire and behaviours.
Access the full resource for Section 3 Staff conduct and attire
There were several specific staff requirements which arose as the COVID-19 pandemic progressed to further implement safe processes and reduce transmission risk for staff, residents and community.
These were enforced through the Chief Health Officer’s Directions with compliance managed by the site.2
These are identified as:
- Provide a level of information upon employment required for use in contact tracing: first and last name, employer, telephone number, address or other contact means, dates and times of working.
- Restriction to only work at the quarantine facility with requests to work in an additional work places to be considered by the CHO. In certain situations, this extended to volunteer work.
- Anyone moving between facilities must have a negative swab before going into another health facility.
- All staff onsite to be up to date with (COVID-19) vaccinations and provide evidence of this.
- All staff to undergo viral screening within 2 hours of site arrival, every time they enter the site (this extended to visitors and contractors).
Quarantine staff have a responsibility to keep the workplace safe from disease transmission and this means self-responsibility in cases where they are unwell, positive with viral infection or possibly infected.
If an unwell staff member attends work they can infect the whole team they work with leaving the facility short staffed and potentially compromised in providing adequate resident care.
Mandatory viral screening and vaccination is one process to mitigate this risk as well as well as ensuring staff do not come to work if they are unwell. Standard precautions in work practices are required to be applied to everyone regardless of their perceived or confirmed infectious status and ensure a basic level of infection prevention and control.
Standard precautions:
- Hand hygiene
- Physical distancing
- Stay at home if unwell and seek advice if viral screening (swabbing) is required.
It is the responsibility of the health employee to report sickness and/or an inability to attend work by calling or texting and notifying the team they work in and their direct line manager and the expected day of return. It is expected that all staff will make all reasonable effort to advise their manager as soon as reasonably practicable on any day of absence from their employment. For staff working in a quarantine facility, infection control is paramount and absences need to be considered to determine if it will affect site operations (i.e. spread of communicable disease/ transmission).
As a supportive staff measure facilities may consider permitting positive staff who are unable to safely isolate at home to quarantine onsite with residents at no cost. Further instructions on managing staff who test positive onsite have been provided in Section 2 Infection Prevention and Control.
Quarantine and isolation facilities have a duty of care for their staff to ensure they feel safe and supported within their work environment. This can be challenging in a pandemic response, particularly in the early stages when there is often pressure to work fast in establishing systems and processes. At this point effective communication channels are still being established and many initial strategies were rapidly reacting to change with staff working long hours in stressful circumstances.
In a staff survey conducted with the Centre for National Resilience Workforce, the survey question related to staff rating their employment satisfaction received positive feedback with 80% agreeing they would have stayed longer if provided the opportunity and 95% would work at a quarantine isolation facility again. In addition, 86% of staff felt they had gained new skills which would be useful for their future career pathway.
This section presents approaches the quarantine facility can utilise to enhance staff mental health and well-being.
Contracting organisations (private and non-government) into the quarantine workforce is a positive strategy to ensure all aspects of the site processes can be met.
This provides an opportunity for employment and financial support of organisations when service provision can be negatively impacted due to pandemic emergency response strategies (such as lockdowns of services and non-essential workforces). It is important this workforce is provided the education and training to ensure they are safe whist working on site and understand they are bound by the policies and procedures of both their employer and the quarantine service.
Site rules implemented for site contractors:
- All staff and contractors entering the quarantine facility must undertake viral screening every day that they are onsite.
- All staff and contractors entering the orange zone MUST have undergone Site Induction Training conducted by the Education Team and Work Health Safety Officer including personal protective equipment (PPE) donning and doffing procedures prior to their first entry to the zone.
- All staff and contractors entering the zone must wear PPE to protect themselves from disease transmission. This means surgical mask, safety goggles or shield and gloves.
- Equipment required to complete maintenance and repairs can be transported into the orange zone on a trolley or buggy as necessary.
- All equipment entering the orange zone will need to be cleaned to an infection control standard prior to leaving the orange zone.
- Staff and contractors working at the HSQF site are required to adhere to their profession specific work health and safety requirements at all times including required personal protective equipment.
- Once within the orange zone and at the worksite it is permissible to place a temporary barrier around the work site and if residents are clearly excluded from that area, usual work health and safety PPE can replace the infection control PPE required in the rest of the orange zone. This is only allowed in the delineated work site and any movement from this site requires infection control PPE to be reapplied.
The collaboration of the quarantine and isolation facility with non-government organisations (NGO) is an essential part of the site function and resident support.
The health and wellbeing of residents in quarantine can be greatly assisted with the inclusion of NGO support and this presents a reciprocal benefit with site funding provision for NGO services.
The size and internal capabilities of the quarantine and isolation facility will directly influence the extent of NGO services required. For assistance with resident care (with a focus on their safe exit from the facility into the community), this should include social and welfare support such as financial, housing, domestic violence support and transport. For Humanitarian residents, there should be automatic inclusion of refugee services initiated by DFAT.
Examples of NGO collaboration at the CNR included (but was not limited to):
Melaleuca Refugee Service: this organisation linked with humanitarian residents and provided assistance with their trauma recovery and integration into Australia.
Save the children: in a collaborative agreement this organisation provided children’s pack kids packs and assisted with the family support of humanitarian and repatriated residents.
Anglicare: this organisation was linked with disadvantaged or vulnerable resident whilst they were in quarantine to provide assistance for residents on exiting the facility.
Saltbush Social Enterprises: provision of counselling and wellbeing and other programs for Aboriginal and Torres Strait Islander residents.
Larrakia Nation – collaborative management for First Nations Peoples (lack of accommodation)
Careflight / Royal Flying doctors – transportation for expatriates, remote communities and medical emergencies
References
- Northern Territory Government. (2023). Department of Infrastructure, Planning and Logistics.
- CHO Directions. COVID-19 Directions (No. 53) 2021: Directions for Quarantine Workers. Northern Territory of Australia.
Content acknowledgement
Content in this resource has been created and, in some cases, directly copied with permission from documents and resources owned and prepared by the Northern Territory Government, Department of Health, Centre for National Resilience, Howard Springs Quarantine Facility and the National Critical Care and Trauma Response Centre.
Reference this webpage (APA style guide)
To reference the webpage:
Charles Darwin University. (2023). Pandemic Quarantine Facility Guide. Top End Academic Health Partners. https://quarantine-guide.cdu.edu.au/
To reference a webpage document:
Charles Darwin University. (2023). Section 3 Health workforce: Nursing Workforce. Top End Academic Health Partners. https://quarantine-guide.cdu.edu.au/wp-content/uploads/2023/05/Section-3-Nursing-Workforce.pdf
Pandemic quarantine facility guide abbreviations and full reference list.
